Research has found that both Type 1 and Type 2 diabetics are deficient in thiamine (Vitamin B1), however typical diagnostic methods for measuring thiamine status will not always reveal this deficiency.
Why are they deficient? One reason is because they have altered gut bacteria behavior which produces less thiamine. However it has also been found that diabetic patients dump (excrete) a high amount of thiamine in their urine via the kidneys.
Why does this matter? Thiamine is required for proper glucose metabolism, for insulin synthesis and secretion, for the health and survival of pancreatic beta cells (which produce insulin), and so much more.
While taking supplemental insulin helps prevent hyperglycemia and the negative effects of having high blood sugar, it does not solve the problem of severe, chronic thiamine deficiency, which is why complications of diabetes can still occur despite the use of insulin.
Thiamine deficiency in and of itself can lead to encephalopathy, cardiovascular disease, and many other manifestations of chronic illness.
Thankfully, the neurological and cardiovascular complications of diabetes, and more, can be remedied by supplementing with high doses of thiamine.
But why do diabetics dump so much thiamine in their urine?
It is possible that one of the root causes of type 1 diabetes may be related to the bioaccumulation of toxic metals in the pancreas (via exposure to lead for example) which damages and kills beta cells. In defense, cells may use up thiamine in order to detoxify and remove the metal via the kidneys, as thiamine is able to form complexes with lead and safely remove it from the body.
Sources and additional details, below.
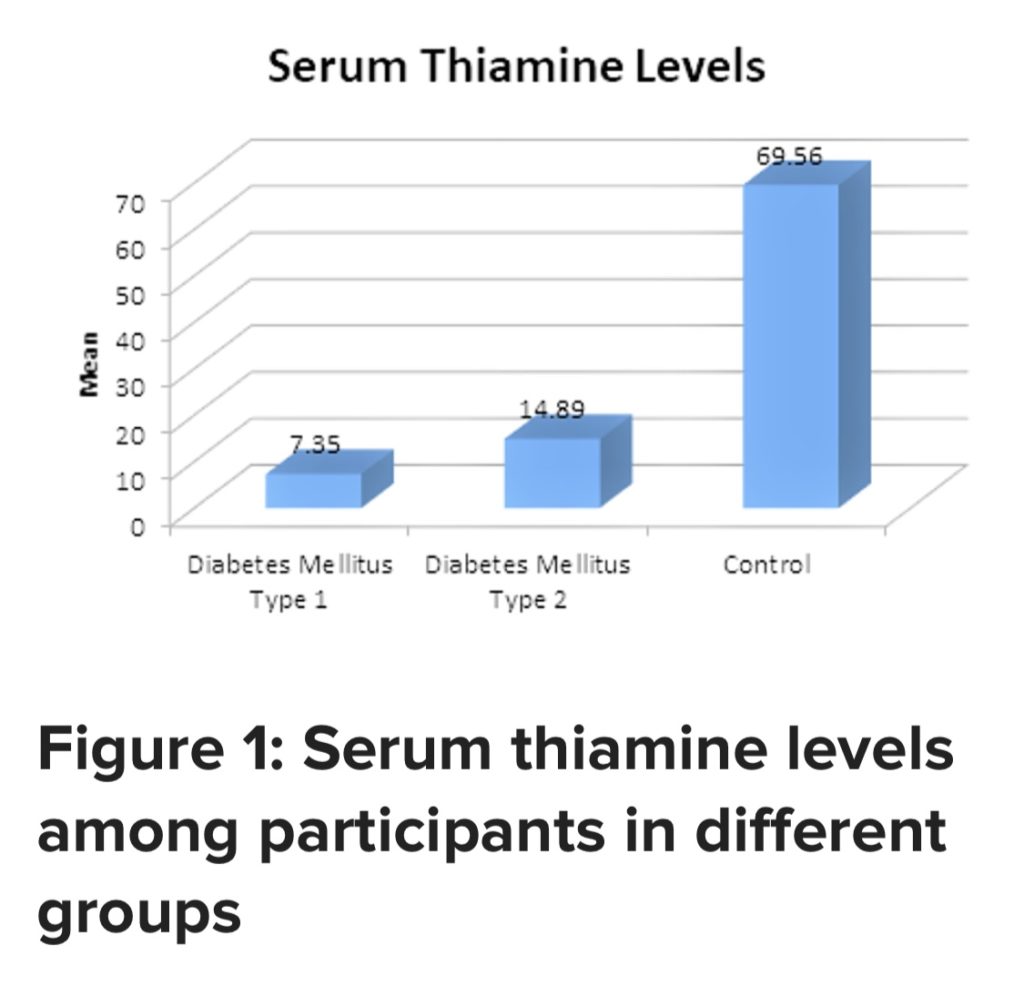
Type 1 & Type 2 Diabetics are severely deficient in thiamine.
“Plasma thiamine concentration was decreased 76% in type 1 diabetic patients and 75% in type 2 diabetic patients,” compared to normal controls. https://link.springer.com/article/10.1007/s00125-007-0771-4
“Low plasma thiamine level was noted in type 1 diabetic patients.” https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3376872/#!po=0.819672
“The plasma content of [thiamine] in type 1 diabetic patients…was significantly lower when compared with that measured in six age-matched normal subjects…” https://pubmed.ncbi.nlm.nih.gov/10436256/
“Thiamine deficiency is common in children with diabetic ketoacidosis…” https://journals.lww.com/pccmjournal/Abstract/2015/02000/Low_Thiamine_Levels_in_Children_With_Type_1.3.aspx
Thiamine deficiency in diabetes is not always apparent when using typical testing methods.
“Thiamine deficiency was not detected by the conventional indicator of thiamine status…”
“Plasma deficiency of thiamine in diabetes was masked in erythrocytes [blood cells]” https://link.springer.com/article/10.1007/s00125-007-0771-4
Diabetic patients have altered gut flora behavior.
“The gut bacteria in those with type 1 diabetes created a deficiency of Vitamin B1…” https://www.diabetesdaily.com/blog/gut-bacteria-changes-in-type-1-diabetes-causes-vitamin-b1-deficiency-318146/
Diabetic patients waste/dump thiamine via their kidneys.
“Renal clearance of thiamine was increased 24-fold in type 1 diabetic patients and 16-fold in type 2 diabetic patients.” https://link.springer.com/article/10.1007/s00125-007-0771-4
Thiamine is required for proper glucose metabolism.
“Thiamine (vitamin B1) is an essential cofactor of several enzymes involved in carbohydrate metabolism and published data suggest that thiamine metabolism in diabetes is deficient.” https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4058733/
“Thiamine plays an important role in the regulation of glucose metabolism and pancreatic beta-cell functioning.” https://pubmed.ncbi.nlm.nih.gov/10436256/
Thiamine is required for insulin synthesis and secretion from cells.
“Thiamine deficiency leads to a marked impairment in insulin synthesis and secretion.” https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3376872/#!po=5.64516
Thiamine is required for proper function and survival of pancreatic beta (β) cells.
“Beta cells are unique cells in the pancreas that produce, store and release the hormone insulin.” https://www.diabetes.co.uk/body/beta-cells.html
“Excessive apoptosis [death] of the pancreatic beta-cell has been associated with diabetes.” https://diabetes.diabetesjournals.org/content/50/suppl_1/S44.short
“Pancreatic β-cell apoptosis [cell death] is [a] pathological feature that is common to both Type 1 diabetes mellitus (T1DM) and T2DM.” https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4978108/
“High glucose modulates the balance… toward apoptosis, thus leading to β-cell death.” https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4978108/
“Vitamin B1 (thiamin) is indispensable for normal function/health of pancreatic cells due to its critical role in oxidative energy metabolism, ATP production, and in maintaining normal cellular redox state. Low intracellular level of thiamin leads to acute energy failure and oxidative stress; it is also known to lead to impairment in the function of mitochondria. At the organ level, [in non-diabetic patients] the pancreas contains high levels of thiamin, and deficiency of this vitamin leads to impairment in its functions. The pancreas cannot synthesize thiamin endogenously, and thus, must obtain the vitamin from circulation.” https://grantome.com/grant/NIH/R01-AA018071-09
“In addition, a reduction in intracellular thiamin leads to apoptosis [cell death].” https://journals.physiology.org/doi/full/10.1152/ajpgi.00092.2009
“…impairment in cellular thiamin accumulation and the development of localized thiamin deficiency in pancreatic beta cells (and other affected tissues) . . . leads to derangements in cellular metabolism, cell stress, and apoptosis.” https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2711754/#!po=8.78378
Thiamine deficiency enhances the damaging effects of hyperglycemia.
“Decreased availability of thiamine in vascular cells in diabetes exacerbates metabolic dysfunction in hyperglycaemia.”
“The deficiency of thiamine in clinical diabetes may increase the fragility of vascular cells to the adverse effects of hyperglycaemia and thereby increase the risk of developing microvascular complications.” https://link.springer.com/article/10.1007/s00125-007-0771-4
Thiamine deficiency is a risk factor for cardiovascular disease.
“…intravenous thiamine administration resulted in improvement of cardiac functions and hemodynamic features.” https://www.sciencedirect.com/science/article/abs/pii/S0939475318302011
Thiamine deficiency leads to neuropathy and neurodegeneration.
“…thiamine deficiency results in significant nervous system pathology…” https://link.springer.com/article/10.1007/BF02080928
“…neurological features include impaired reflexes and symmetrical motor and sensory deficits in the extremities. Loss of myelin is seen without any acute inflammation.” https://www.ncbi.nlm.nih.gov/books/NBK537204/
Thiamine protects against complications of hyperglycemia and diabetes.
“Thiamine definitively has a role in the diabetic endothelial vascular diseases (micro and macroangiopathy), lipid profile, retinopathy, nephropathy, cardiopathy, and neuropathy.” https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3376872/#!po=0.819672
“Correction of the low plasma thiamine concentration with thiamine supplements may decrease the risk of microvascular complications in diabetes.” https://link.springer.com/article/10.1007/s00125-007-0771-4
“Thiamine administration can prevent the formation of harmful by-products of glucose metabolism, reduce oxidative stress and improve endothelial function.” https://pubmed.ncbi.nlm.nih.gov/21564442/
“Optimization of thiamin level appears to have the potential of preventing diabetic retinopathy and blocking tissue damage caused by hyperglycemia of diabetes.” https://journals.physiology.org/doi/full/10.1152/ajpgi.00092.2009
Patients with Thiamine-responsive megaloblastic anemia syndrome (TRMA) typically develop diabetes and require insulin, yet are able to reduce or stop taking insulin with high doses of thiamine.
“Thiamine-responsive megaloblastic anemia syndrome (TRMA) is an autosomal recessive disorder characterized by megaloblastic anemia, progressive sensorineural hearing loss, and diabetes mellitus.” https://www.medscape.com/answers/204930-69697/what-is-thiamine-responsive-megaloblastic-anemia-syndrome-trma-and-how-is-it-diagnosed
“Supplementation of TRMA patients with high doses of thiamin brings about a marked improvement in the clinical symptoms of the disease including a reduction or cessation in the need for exogenous insulin.” https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2711754/#!po=8.78378
Chronic lead exposure is a risk factor for insulin resistance and diabetes.
“Chronic exposure to lead can disrupt glucose homeostasis by affecting pancreas and liver mainly through induction of insulin resistance.” https://www.sciencedirect.com/science/article/pii/S1382668914002592
“In an earlier study with factory workers in the United Arab Emirates significant positive correlations between blood lead levels and fasting blood glucose were observed, suggesting a possible link between lead exposure and diabetes.” https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6161143/
Thiamine protects against lead toxicity.
“…thiamin interacted with [lead] in some way to prevent tissue accumulation, thus preventing clinical signs and death.” https://www.sciencedirect.com/science/article/abs/pii/0041008X81904646
“…thiamine enhances elimination of [lead] from the body and this feature may be beneficial in chelation therapy.” https://pubmed.ncbi.nlm.nih.gov/1755021/
“…thiamine can reduce blood lead levels and further reverse early biochemical markers of lead toxicity.” http://repository.ias.ac.in/96348/1/Therapeutic_potential.pdf
“The liver, kidney, and blood of rats receiving supplemental thiamine also contained significantly less [lead] than the other two treatment groups given [lead]-containing water. The protective effect of thiamine against [lead] toxicity may be attributed to its interference with retention of the metal in body tissue, possibly resulting from the formation of excretable thiamine-lead complexes.” https://pubmed.ncbi.nlm.nih.gov/24254360/
Lead exposure negatively impacts gut flora.
Multi-Omics Reveals that Lead Exposure Disturbs Gut Microbiome Development, Key Metabolites, and Metabolic Pathways https://pubs.acs.org/doi/abs/10.1021/acs.chemrestox.6b00401
Supplementation
Form: Thiamine hydrochloride (HCl).
Important notes:
Benfotiamine is a lipid soluble form of thiamine which is considered to be more easily absorbed, but may not have the same ability to detoxify and remove lead from the body.
Consider supplementing with magnesium as well if you intend to supplement with thiamine.
“The active form of [thiamine] together with magnesium is an essential cofactor of several enzymes important for carbohydrate … and amino acid … metabolism.” https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4058733/
High-dose thiamine supplementation (3 x 100mg/day) improves glucose tolerance in hyperglycemic individuals: a randomized, double-blind cross-over trial https://pubmed.ncbi.nlm.nih.gov/23715873/
“Quality of life was enhanced by providing thiamine supplements. Blood pressure and weight were lower after thiamine supplementation (10mg/day).” https://academic.oup.com/ajcn/article/66/4/925/4655987?login=true
Additional reading:
The Impact of Thiamine Treatment in the Diabetes Mellitus https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3376872/
A Review of the Biochemistry, Metabolism and Clinical Benefits of Thiamin(e) and Its Derivatives. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1375232/#!po=0.510204
Pharmacokinetics of high-dose oral thiamine hydrochloride in healthy subjects https://link.springer.com/article/10.1186/1472-6904-12-4